two boys, two totally different births. {Tampa Bay Doula}
This story comes to us from a lovely family Charlie had the honor to walk with through their second birth journey as their doula. Sarah's stories are that of trauma, heartache, determination, and ultimately strength. Through everything, this family has navigated bumps in the road with so much knowledge and peace knowing that they were in control (even when they were not!) We love to point out that this also shows that doula support is not just for unmedicated vaginal birth! Doulas support families through all sorts of events surrounding childbearing and parenthood. Thank you to Sarah and family for having the courage to share their story- we know it is inspiring to many!
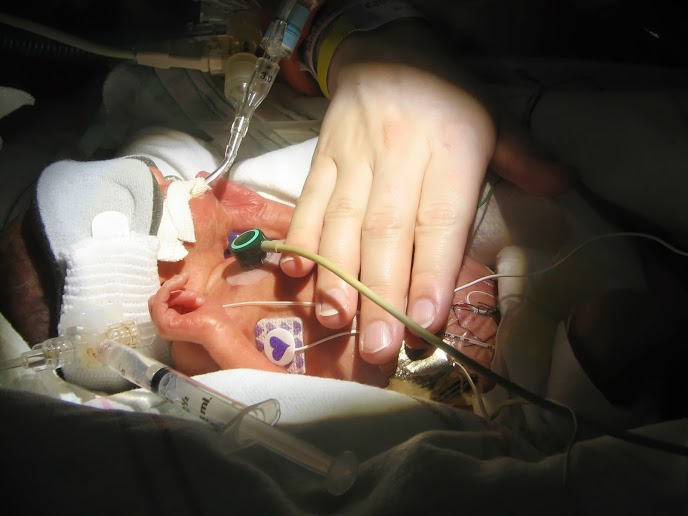
The day my first son was born was one of the most exciting and terrifying days of my life. 48 hours before he was born, I started having contractions. I was just 28 weeks pregnant. Magnesium sulfate was given to stall labor, causing me to become paralyzed and vomit, therefore aspirating it into my lungs. The side effects were horrific- skin burning like I was on fire, blurred vision, feeling doped up. What made it worse was that I had been having contractions for a month but the doctor’s office brushed me off. Even went to the hospital a week before my son was born and was sent home without an ultrasound. I felt betrayed.
After an ultrasound we were told there was something terribly wrong with the baby. He had a birth defect and probably Beckwith Wiedeman syndrome. After an internet search, my husband came back in tears telling me it meant mental retardation and cancer. We were heartbroken to hear that not only would our son be dealing with prematurity, but would also be battling a cruel disease. We were just 24 years old. Even though I was doped up from the magnesium, and this was my first child, who may not survive, I was repeatedly asked if wanted my tubes tied. I found this terribly disrespectful. Luckily the docs were able to get me the 2 shots of steroids that greatly improve a premature baby’s chance of surviving. At 5 cm they gave up on preventing the birth, as my lungs were filling with fluid from the magnesium. 48 hours of pain, nausea, burning, terror, darkness, inability to breathe. I needed a break, and got an epidural and pitocin. I was not told of any of the risk of these interventions. They dosed the epidural too high and I was completely numb. When it was time to push, I couldn’t do a good job and was threatened with a c-section if I didn’t push well for them. Not sure what happened, but soon I was given an episiotomy and they pulled out the baby with forceps. Our son was born weighing 3lbs 7oz. I wasn’t allowed to see him as they rushed him to a table to intubate him. My husband watched this. Then they rushed him to the NICU. 3 hours later we were allowed to see him in his little incubator box, but not to hold him.
The next day he was transferred to a children’s hospital for emergency surgery. He had been born with a ruptured intestine. A week later I got to hold him. At one month old I finally got to do skin to skin kangaroo care. Due to his intestines being unhappy, he had to be tube fed so I pumped milk for him. At 3 months old I finally was able to put him to my breast. I took home a very sick baby. His medical and developmental problems took a long time to recover from.
We had wanted more children but our terrible birth experience and fear of having another sick child made us wary. I did tons of research, took time to get my body in tip top shape, detoxed, ate lots of clean food, and took a lot of vitamins. I was feeling better than ever, and some of my own health issues were greatly improved. Genetic testing showed our son did not have any known genetic disease (including the one they were sure he had). We felt we were strong enough to go through another pregnancy and we could deal with whatever nature handed us. Our son had also made an amazing recovery.
I got pregnant and started seeing a high risk OB group. They took my concerns seriously and I felt safe with them watching over me. When I started bleeding they had me come right in for an ultrasound and it was a minor sub-chorionic hemorrhage, which they followed until it cleared. I went to Tampa Bay Birth Network’s Childbirth Options seminar. They started doing a visual demonstration of labor interventions, taping strings on a volunteer to demonstrate how one intervention can snowball into many. I felt sick inside. I had to get up and go hide in the bathroom because I couldn’t stand to watch. I had no idea I felt this strongly about my first birth. Later I talked to some kind women, who pointed me towards ICAN as a resource for someone who had had a traumatic birth. I started attending meetings and educating myself about natural birth. I had decided that with my child’s history of developmental delays, medicated childbirth was risky, and I wanted a homebirth. I picked out a midwife and we decided that if the 20 week ultrasound looked clear, I would start seeing her for my prenatal care. I could have monthly ultrasounds just like the high risk doctors were planning to do. If anything it would probably be better if any issues came up, since my concerns would be addressed by one practitioner instead of being filtered through many nurses and a group of OBs.
At the 20 week ultrasound it was discovered that I had a complete placenta previa. I started to tear up since I knew this was dangerous and meant a c-section and possible premature birth. The doctor said “don’t worry, they often shift away from the cervix”, so we started doing regular ultrasounds to see if the placenta had moved.
I was also having frequent nightmares. Uterus rupturing, NICU stays, dead fetuses, anything my mind could come up with to haunt me. I reached out to the network of women who were supporting me. I went to a birth healing workshop which brought me peace. I also shared my story at a birth story circle. My husband and I went to 10 weeks of Bradley classes. We learned how to advocate for myself and our baby. Knowing my husband had also been traumatized at our first birth, I wanted another advocate there so my husband and I could relax and enjoy our baby’s birth. I wanted a doula who had been at a lot of hospital births and who was very passionate and experienced, and that was Charlie Rae. The ultrasounds showed the placenta was stubbornly clinging to my cervix. I resigned myself to a planned c-section at 39 weeks. The wonderful women of ICAN helped me write a birth plan for a gentle c-section. More than anything, I wanted to hold my baby right away, I didn’t want anyone to take my baby away from me.
I had a consult with anesthesia ahead of time to discuss my chronic low blood pressure, need for a blood transfusion, delayed cord clamping, and immediate skin to skin. It’s normal for blood pressure to drop from the spinal, so they would give me extra IV’s of fluid before the surgery. Blood pressure drops can cause nausea and vomiting. I did not want to vomit and lose out on skin to skin. I wanted to avoid a transfusion. One liter was the average blood loss during a section (mine turned out to be 700cc’s), and this was acceptable because a woman’s body has extra blood during pregnancy in case some is lost. They said delayed cord clamping was not rare at that hospital, and the anesthesia doc had seen it several times. They said there wouldn’t be a problem with immediate skin to skin, although with the drapes I probably could not breastfeed in the OR. The baby would go on my upper chest. They said they would use warmed blankets on top of me to assist in keeping us both warm and they also have a device similar to a blow dryer if we got really cold. I was told the nursery staff (the ones in the OR in charge of the baby) would be the biggest obstacle. So I had a little chat with the nursery team. They seemed a little resistant to the idea, and also said there would need to be extra staff in the OR to stay with the baby if he didn’t go to the nursery. Normally if they take the baby to the nursery right away, and there are lots of c-sections, they only need one nursery team member to cover all the babies. I also called up the head of the OB department and OK’ed my birth plan with her, focusing on the skin to skin issue. She said it was fine as long as we were both stable. I ended up needing to quote her to get my skin to skin.
Words cannot express how happy I was to feel frequent movement of the baby (didn’t happen the first time), see a healthy baby on the ultrasounds, and approach 40 weeks. I had a celebration when I passed 28 weeks and 36 weeks.
My surgery was scheduled for a Monday. The Wednesday before, my body had other plans. At 38 weeks, my cervix must have started to dilate. I was sitting on the couch when I suddenly felt a ton of movement and then a wet spot. I was horrified to find I was bleeding heavily. Most disturbingly, I didn’t feel any more movement. It was 1am. I woke up my husband and son, grabbed the hospital bag, threw a towel between my legs, and we were off. The hospital was 15 minutes away. I called ahead to the hospital, called Charlie, called my in-laws to pick up our older son at the hospital. I was shaking badly from the fear that the baby was being deprived of oxygen as I still hadn’t felt movement. My husband dropped me off, I walked into the labor ward, and the woman at the desk told me to have a seat in the waiting room. I told her “no, I want someone to check the baby’s heart beat right away and to get me a freaking wheelchair because I am hemorrhaging”. They actually listened to me then, and I was relived to see the baby’s heartbeat was steady. By the time the doc came in, the bleeding had stopped. But they said it would be wise to go ahead and do the section now. So I consented. Luckily I had a copy of my birth plan in my purse, since I knew previas were liable to start bleeding at any time. The hospital staff said my husband would have to stay with my older son and miss the birth unless we had someone to watch him. Thankfully Charlie got there in time and my in-laws picked up my son. The staff was kind to me and respected my birth plan. They promised to delay cord clamping and do immediate skin to skin provided baby and I were stable, and allowed my doula to come n the OR also. It was almost nice that it was 3am because I was the only patient and they could take more time with me. I reminded them of my low blood pressure and I had a few bags of fluid first.
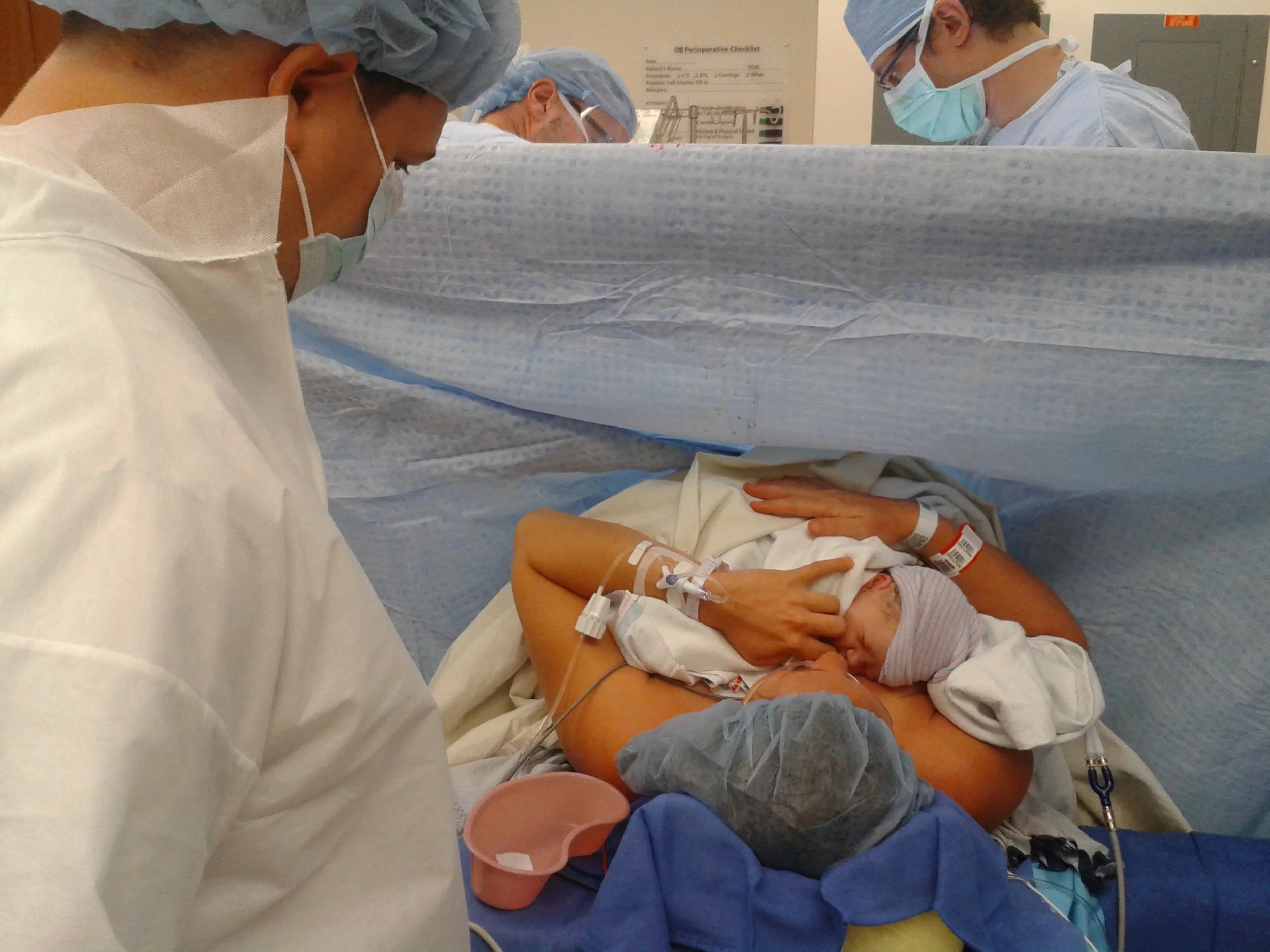
The spinal went in perfectly. Thankfully it gave me a high, my body became warm and numb, and I finally stopped shaking from fear. My blood pressures dropped 4 times, making me feel deathly ill, so they gave me more fluid. When my husband and Charlie came into the OR in marshmallow suits, I was smiling. I was so excited to meet my baby. I was not nervous as they started cutting. The baby was rather large and it took a good 5 minutes of tugging to get him out, I was pretty bruised afterwards. It felt like the wind was getting knocked out of me. Charlie was there talking me through it. They held him up and announced “it’s a boy”, which is what we had guessed. He went to the warming table for assessment. I started to ask they give me the baby. My husband, then Charlie went over to the table to ask. Obviously he was healthy and doing well. They dried him off and stimulated him. We all kept asking, even the surgeon said something like “just give Mom her baby already”. I told the nursery staff I had OK’ed immediate skin to skin with the head of OB. My doula repeated this. I think it was about 5 minutes but I finally got to hold him. The nurses handed the swaddled baby to my husband. Charlie and my husband quickly took off the blankets and helped to put his diaper clad body on my upper chest. He was so beautiful. He smelled so good. He was covered in vernix. He was crying, and my breasts were not really accessible due to the drapes, so I put my finger in his mouth. I held him for a magical 5 minutes when the horrible feeling of nausea and low blood pressure came on again. I passed him off to my husband and I got more fluid. We had originally decided against taking him out of the OR to the nursery, but at that point I needed to rest. I think it took another 20 long minutes to finish the surgery. In the recovery room they brought me the baby and I was able to breastfeed right away. I was gloriously happy to have a healthy baby in my arms.
The surgeon and his assistant (a resident) both agreed to delayed cord clamping. I did not hear them count during the surgery after the baby came out. I asked them afterwards and they said they did it, but it is not in the surgical report. Looking back, I am also glad they used a nasal cannula; as at my first birth I had an oxygen mask on, and it made me claustrophobic, and made it hard to advocate for myself.
We were able to bond successfully right away. Breastfeeding was established, despite pain med side effects and a lip tie. The drugs made my eye crossing act up, so I needed my prism glasses to get him latched on. I got a few extra bags of fluid. My doula brought me a smoothie with placenta medicine. I was given adequate pain meds, had the catheter removed, and started walking right away. Friends brought me wonderful healing food. The surgeons did an excellent job and they sent me home on day 2. My incision healed beautifully. Everything was so right. With my first son I struggled with depression for a long time, not classical postpartum depression, but more of a post-traumatic depression. With this baby, I did not have depression. I think it was still hard on my husband, because he spent so much time supporting me afterwards and I don’t know if he really believed things were really going this well. But as the months have gone on, it’s feeling more real. I have a healthy baby, and I am physically and mentally healthy. Thanks to the advocacy of my community of women, my husband, and myself.
Here is the birth plan I used:
Cesarean Birth Plan
I had a traumatic birth with my first son. He was extremely premature and had a birth defect, and I had a very difficult time breastfeeding him. I appreciate you taking the time to read this. Please help me to have a less scary birth and achieve my breastfeeding goals.
During Surgery:
Surgeon:
- Please reinforce my uterus with double sutures and use dissolvable stitches for closing me up.
- Please no casual conversations, as quiet as possible, no extra students/residents.
- Please hold baby up for me to see as soon as Baby's born.
- Delay cord clamping 1-2 minutes.
- Placenta will go to doula instead of pathology.
Anesthesia:
- I would like to have my doula in the OR with Dad and I to keep us both calm.
- EKG leads away from anterior chest wall where the baby will be placed.
- IV placed on left (non-dominant) hand.
- Warm blankets during surgery.
- Give extra fluids during/ after surgery due to history of low blood pressure/ vagal reactions.
- Would like dextrose in fluids, no lactated ringers- family history of mitochondrial disease.
- No sedatives after birth. I want to remember my Baby's first day of life.
- Doula will photograph c-section after OK is given.
Nursery Team:
Please note: this has already been approved by Ms. X head of OB, the OB surgeon, and an anesthesiologist, provided Mom and
Baby are doing well.
- Nursery team member positioned at the top of the bed beside my head.
- Lay wet baby on Mom’s chest for drying instead of warmer.
- First set of vitals will be done on Mom’s chest.
- Towels/ blankets placed on top of Mom/ Baby instead of swaddling.
- Anesthesia will assist in keeping baby warm with warm blankets/ heater.
- Mom will hold Baby while Baby is being foot printed, getting bracelets on, and during paperwork.
- Delay weighing and measuring baby until surgery is finished.
- Newborn vitals will be done while baby is on mom’s chest.
- No Eye Gel, no vitamin K shot. Mom will sign the waiver ahead of time.
- Baby is NOT to be separated from mom unless there is a medical emergency with the baby, baby will stay in OR with Mom and Dad even if Mom vomits.
- Dad and Doula can assist with keeping baby on Mom’s chest to free up Nursery Team member.
- Delay Baby's bath until the evening after Baby is born, Mom and Dad will bathe baby.
Baby/Postpartum Care Plan:
§ I
will keep Baby with me at all times, Dad and Doula will assist me.
§ Once
back in our room to recover and been checked as stable, we would like to be
alone with Baby to nurse.
§ If
someone arrives to visit, please check with Mom or Dad as to whether we are up
for company before allowing them in our room.
§ I
am willing to be up and walking as soon as possible, I would like my Catheter
out ASAP after surgery.
§ Delay
Baby's bath until the evening after Baby is born, Mom and Dad will bathe baby.
§ I
will be nursing on demand.
§ No
routine bloodwork (blood sugar, bilirubin) except for newborn screening
(newborn screening while breastfeeding).
§ No
formula or supplements, family history of food allergies
§ No
Hepatitis B vaccine; mom and dad are negative for Hep B.
§ Do
not wake me for routine checks as I have a sleep disorder and need all the
sleep I can get.
§ Mom
has food allergies.